Key Takeaways
- 1Labiaplasty recovery is shaped by the vulvar region's unique vascularity and cellular structure, leading to faster and distinct healing patterns compared to other body areas.
- 2Recovery progresses through predictable biological phases, but individual factors such as age, hormonal status, and overall health significantly influence the timeline.
- 3The most intensive healing occurs within the first 48 hours, with substantial progress typically seen by weeks two to three.
- 4Complete structural healing is generally achieved within five to six weeks, while cosmetic maturation and tissue remodelling may continue for several months.
- 5Personalised medical guidance and ongoing follow-up are important during healing and to address individual anatomical variation.
Understanding the Biological Foundation of Labiaplasty Recovery
The vulvar anatomy consists of highly vascularised tissue that responds uniquely to surgical intervention. Medical literature demonstrates that labial tissue contains specialised cellular structures that promote rapid healing compared to other areas of the body.
The biological process of wound healing in genital tissue follows distinct phases, with the initial inflammatory response typically lasting 72-96 hours post-procedure.
For patients asking the practical version of this question, the usual short answer is that desk-based activity often resumes in about one week, while exercise and intimate activity usually need a longer break. The exact timeline depends on the procedure performed, the patient's healing response, and whether the recovery is progressing normally.
The First 48 Hours: Critical Initial Healing Phase
The immediate post-surgical period represents the most intensive phase of the healing cascade. Postoperative care emphasises effective pain management when tissue response is at its peak.
The first two days involve the most significant inflammatory response, which is a normal part of healing. Understanding risks and complications during this critical window helps patients recognise normal healing responses versus concerning symptoms.
Week One: Managing the Inflammatory Response
The transition from acute tissue response to organised healing begins as the initial inflammatory phase subsides. Research shows that sutures typically begin the integration process within the first week, though complete dissolution may take up to three weeks.
The initial seven days represent the critical period for establishing proper wound healing patterns. Adherence to postoperative protocols directly correlates with healing quality and timeline outcomes.
Week Two: Cellular Regeneration and Tissue Adaptation
The second week marks a transition from acute inflammatory response to the proliferative phase of healing. Collagen synthesis accelerates during this period, contributing to structural integrity of the healing tissue.
Individual variation in healing response becomes more apparent during this phase, with some patients experiencing faster tissue adaptation than others.
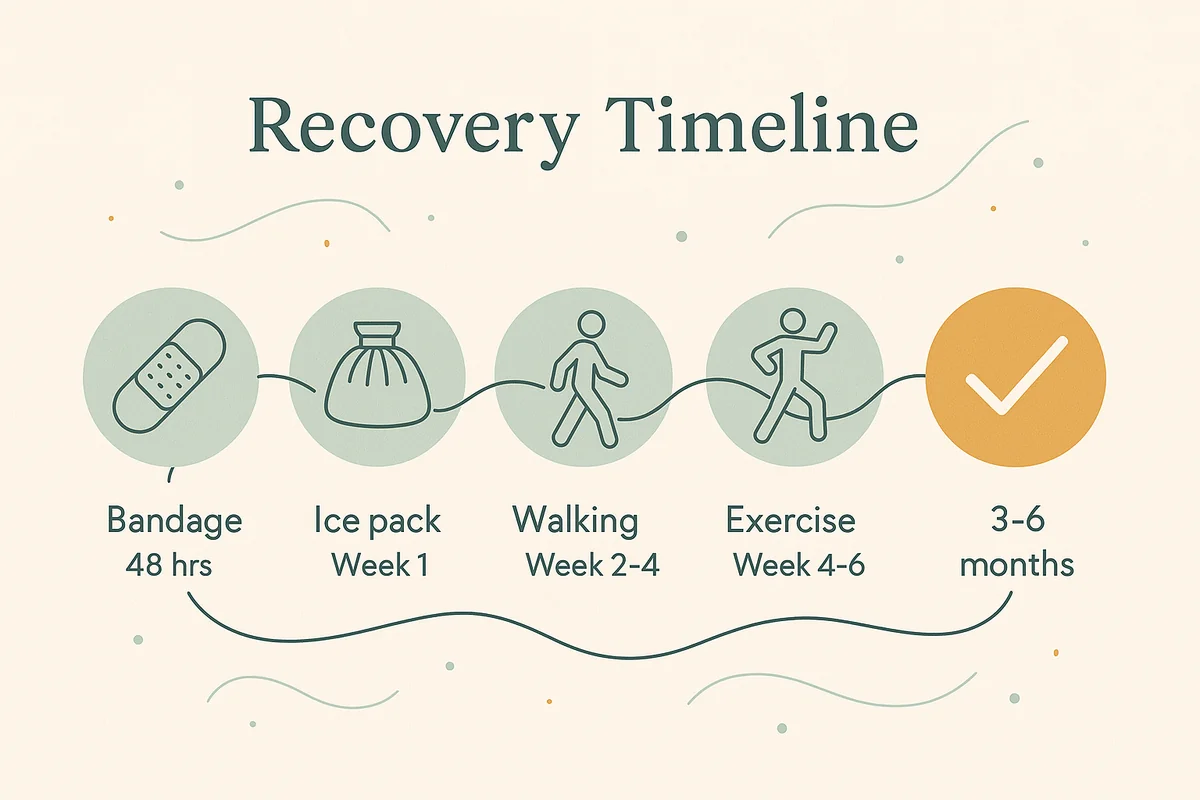
Recovery timeline overview. Individual recovery varies.
Week Three: Structural Integrity Development
By the third week, wound dehiscence risk significantly decreases as tissue strength is supported by ongoing collagen formation and cross-linking. Anatomical studies show that the labial tissue's unique blood supply contributes to the progressive strengthening observed during this timeframe.
Week Four: Functional Recovery Considerations
The fourth week typically represents a significant milestone in functional recovery. The biological processes involved in tissue remodelling reach a level where normal daily activities can often be resumed with appropriate medical guidance. Individual healing timelines vary based on factors including age, overall health, and adherence to postoperative protocols.
Weeks Five to Six: Advanced Healing Phase
Medical literature documents that complete structural healing generally occurs within five to six weeks, though cosmetic maturation continues beyond this timeframe. The advanced healing phase involves ongoing tissue remodelling that affects both functional and aesthetic outcomes. Continued professional guidance through labiaplasty recovery is essential for optimal healing.
Long-term Healing: Months Two and Three
Tissue maturation continues for several months after the initial healing period, with ongoing changes in texture and appearance. Individual factors such as age, hormonal status, and genetic predisposition influence the extended healing timeline, with some patients experiencing continued subtle changes for up to six months post-procedure.
Factors Affecting Individual Recovery Timelines
Anatomical variation significantly impacts healing patterns, with no two patients experiencing identical recovery courses. Factors including smoking, medical conditions, and medication use can substantially alter expected healing timelines. Ongoing professional review remains important throughout recovery.

General activity guidelines. Follow Dr Konrat's specific instructions for your recovery.
Professional Guidance and Monitoring Throughout Recovery
Dr Konrat's approach emphasises comprehensive monitoring throughout the recovery process, recognising that clinical review is essential for identifying normal versus concerning healing patterns.
Your Recovery Begins with Professional Assessment
Each patient's biological factors create an individual recovery experience that requires professional medical guidance. If you're considering this procedure or have questions about recovery, contact our practice to discuss how your individual anatomy and circumstances may influence your personal healing timeline.
Frequently Asked Questions
How long should I take off work after labiaplasty surgery?
Most patients can return to desk-based work within one week, though this depends on your individual healing response and job requirements. Physical jobs requiring lifting or prolonged standing may require 2-3 weeks off.
When can I resume exercise and physical activities after labiaplasty?
Light walking can usually begin within the first week, but vigorous exercise should be avoided for 4-6 weeks to prevent complications. By week three, wound dehiscence risk decreases substantially, but activities like cycling, running, or gym workouts require medical clearance.
What makes labial tissue heal differently from other body areas?
Vulvar anatomy consists of highly vascularised tissue with specialised cellular structures that promote faster healing compared to other body regions. The unique blood supply creates distinct healing patterns, with the initial inflammatory response typically lasting 72-96 hours.
Is it normal to experience swelling for several weeks after surgery?
Yes, swelling is a normal part of the healing cascade and can persist for several weeks. The inflammatory response peaks in the first 48 hours, then gradually subsides. Complete structural healing generally occurs within six weeks, though cosmetic maturation continues for several months.
How do I know if my healing is progressing normally?
Normal healing follows predictable phases, starting with acute inflammation in the first 72-96 hours, followed by cellular regeneration and gradual tissue strengthening. Warning signs requiring immediate medical attention include excessive bleeding, signs of infection, or unusual discharge. Regular professional assessment is essential.